- Blog
- Rough draft outline example
- Rh negative blood type ancestry
- Waifu sex simulator model downlaod
- Waifu sex simulator vr 3-3 models
- Waifu sex simulator patreon models
- Set timer for 2 and 12 minutes
- Life coach wheel
- Garageband free download for hp
- Adobe acrobat xi pro keygen generator
- Free roadblocks games
- Solving quadratic equations worksheet
- Noteburner spotify music converter not parsing
- Calendar template 2018 microsoft word
- Adobe master collection cc 2017 mac torrent
- Graphing on coordinate plane
- Zelda twilight princess gamecube iso download dolphin
- 247 double freecell
- Halion sonic se library
- Wacom intuos paper pro install inkscape
- Syllables picture words worksheet for kindergarten
- Cambridge soundworks 5-1 surround sound rear speakers
- Nexomon extinction cruff location
- Download miracast drivers windows 8-1
- Best crosshair for stretched valorant
- Ring sizer for men
- Softimage 3d resident evil 2
- Openoffice medical brochure template
- 2048 x 1152 banner background gaming
- What was dalton-s atomic theory
- Spinal cord dorsal column stimulator
- Long bodied cellar spider southern california
- Fantasy football draft cheat sheet excel
- Adobe acrobat reader windows 7 free download
- Online sketchpad for stylus
- Calculate degrees of freedom multiple regression
- Apps like notability for windows
- Microsoft office 365 crack download
- Free download klondike solitaire games
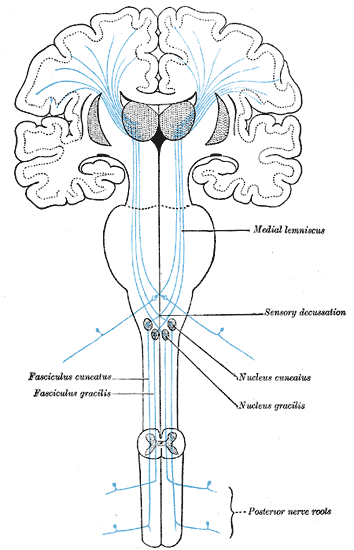
During the trial, the patient complained of discomfort from the SCS (10 Hz). After providing the patient with sufficient explanation, a 1-week SCS trial for the management of pain in the lower limbs was conducted. Lumbar spine magnetic resonance imaging revealed a bulge in the lower lumbar spine disks and mild dural sac exclusion, but no significant spinal canal stenosis (Fig. However, from age 53, the pain in her lower limbs worsened, and she had difficulty in walking. The oral administration of pregabalin, duloxetine, neurotropin®, tramadol, and clonazepam helped ameliorate the pain, and the patient was able to continue with her daily life. She was treated with oral medication and physiotherapy, but had difficulty in controlling her pain thus, she was referred to our department at age 51. In our hospital, the diagnosis was confirmed by the American College of Rheumatology 1990 Criteria. Case presentation Case 1Ī 57-year-old woman who began to feel weakness in her lower legs around the age of 46 and gradually developed generalized pain was diagnosed with FMS by her previous physician. The authors obtained written informed consent from the patients regarding the publication of this case report and the use of related data.

We report two cases in which SCS at 1000 Hz was effective against chronic lower-limb pain in patients with FMS. The pain was alleviated after 1000-Hz stimulation, without irritation therefore, leads and an internal pulse generator (IPG) were implanted in the patients. As we supposed that SCS might be an option to improve the refractory pain that accompanies FMS, we conducted a 1-week, temporary SCS trial. Patients with FMS suffer from refractory chronic pain and limited daily activity. Spinal cord stimulation (SCS) has been reported to be effective for neuropathic and ischemic pain, as well as central pain however, few studies have addressed the effectiveness of SCS for FMS pain. Considering the different mechanisms of pain sensitivity, multidisciplinary treatment programs are recommended to target the peripheral, central, cognitive–emotional, and interpersonal causes of chronic pain. Pharmacological treatment alone is inadequate for most patients who suffer from FMS. This indicates that there may be a problem with the amplification of pain or with sensory processing in the central nervous system (CNS).
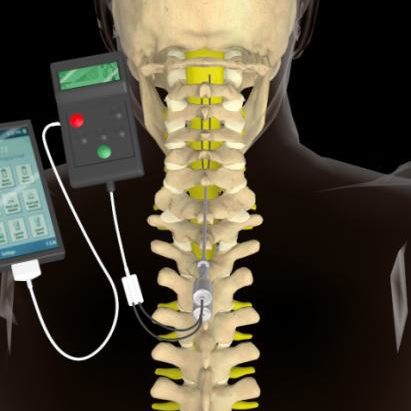
Patients with FMS present a lower pain threshold, which generates a condition of diffuse hyperalgesia and/or allodynia. A diagnosis of FMS is established if the pain is not directly attributable to a nociceptive process in these regions and if there are features consistent with nociplastic pain. It is associated with sleep disorders, cognitive dysfunction, and somatic symptoms. This syndrome is defined as diffuse musculoskeletal pain in at least four of five body regions and in at least three or more body quadrants (as defined by the upper–lower/left–right parts of the body) and axial skeleton (neck, back, chest, and abdomen). Fibromyalgia syndrome (FMS) is a form of chronic widespread pain in the classification of chronic primary pain by the International Classification of Diseases 11th revision (ICD-11).
- Blog
- Rough draft outline example
- Rh negative blood type ancestry
- Waifu sex simulator model downlaod
- Waifu sex simulator vr 3-3 models
- Waifu sex simulator patreon models
- Set timer for 2 and 12 minutes
- Life coach wheel
- Garageband free download for hp
- Adobe acrobat xi pro keygen generator
- Free roadblocks games
- Solving quadratic equations worksheet
- Noteburner spotify music converter not parsing
- Calendar template 2018 microsoft word
- Adobe master collection cc 2017 mac torrent
- Graphing on coordinate plane
- Zelda twilight princess gamecube iso download dolphin
- 247 double freecell
- Halion sonic se library
- Wacom intuos paper pro install inkscape
- Syllables picture words worksheet for kindergarten
- Cambridge soundworks 5-1 surround sound rear speakers
- Nexomon extinction cruff location
- Download miracast drivers windows 8-1
- Best crosshair for stretched valorant
- Ring sizer for men
- Softimage 3d resident evil 2
- Openoffice medical brochure template
- 2048 x 1152 banner background gaming
- What was dalton-s atomic theory
- Spinal cord dorsal column stimulator
- Long bodied cellar spider southern california
- Fantasy football draft cheat sheet excel
- Adobe acrobat reader windows 7 free download
- Online sketchpad for stylus
- Calculate degrees of freedom multiple regression
- Apps like notability for windows
- Microsoft office 365 crack download
- Free download klondike solitaire games
